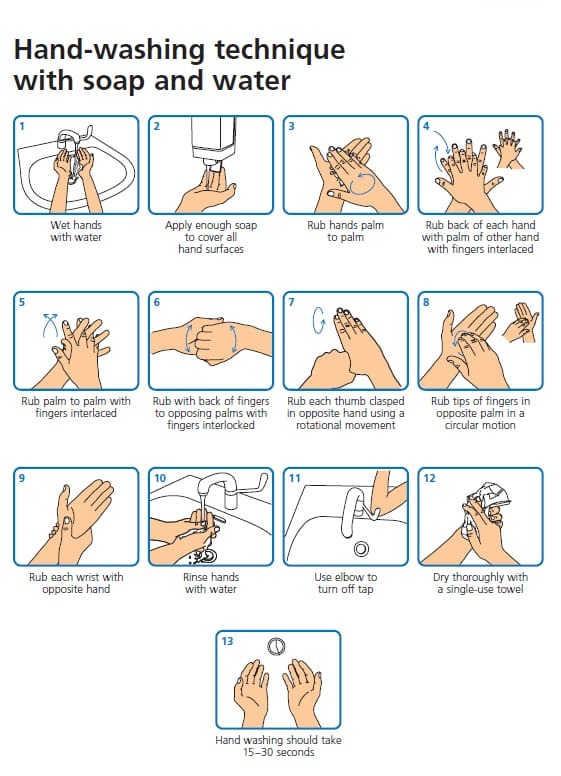
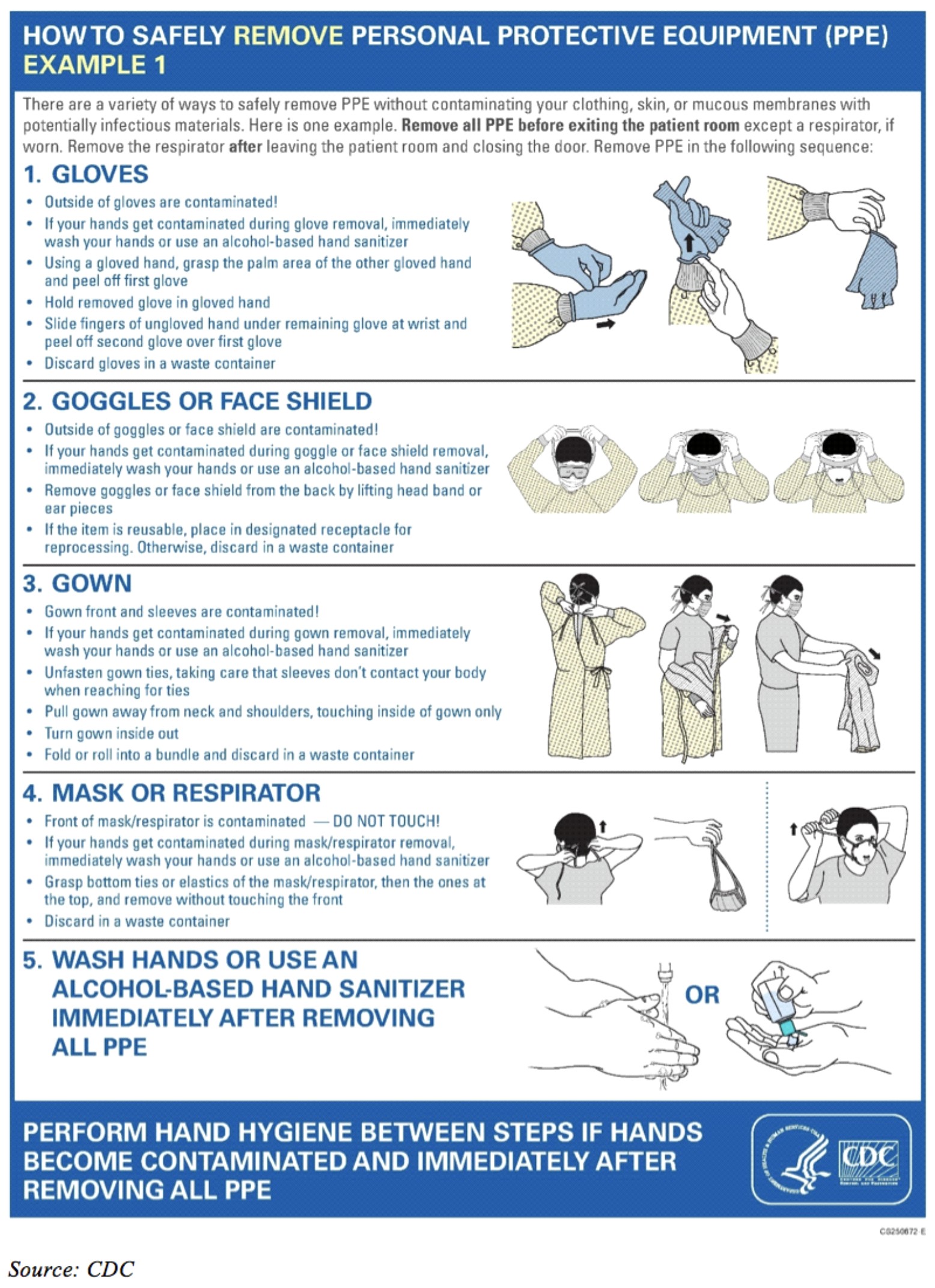
INFECTION PREVENTION & CONTROL GUIDELINES guidelines
Personal Protective Equipment (PPE)
1. Select PPE based on the assessment of risk. The type of PPE used depends upon the level of precaution required (standard, contact, droplet, airborne).
2. The sequence of donning and doffing should be adjusted to specific type of PPE worn.
3. Except for N95 mask/respirator, remove PPE at doorway or in anteroom. Remove N95 mask respirator after leaving patient room and closing door.

When
1. Protective, impermeable gowns or plastic aprons should be worn if potential exists for splashing, splattering or spraying of blood and body fluids (vomitus, feces, urine etc).
2. Do not wear the same gown for care of more than one person.
How?
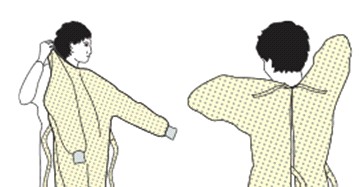
1. Fully cover torso from neck to knees, arms to end of wrists, and wrap around the back.
2. Fasten in back of neck and waist.
When
1. Risk of contact with respiratory secretions (contact and/or droplet and/ or airborne precautions).
2. Risk of transferring bacteria (from mouth and nose) to the potential patient ( lumbar puncture etc).
Aerosol Generating Procedures
1. Intubation, extubation, and related procedures, e.g. manual ventilation and open
airway suctioning (including tracheotomy care and open suctioning with invasive
ventilation).
2. Cardiopulmonary resuscitation.
3. Bronchoscopy (unless carried out through a closed- circuit ventilation system).
4. Surgery and post-mortem procedures in which high- speed devices are used.
5. Dental procedures.
6. Non-invasive ventilation (NIV), e.g. bi-level positive airway pressure ventilation (BiPAP).
7. Continuous positive airway pressure ventilation (CPAP)
8. High frequency oscillatory ventilation (HFOV).
9. Induction of sputum.
10. Collection of lower respiratory tract specimens (e.g. bronchial and tracheal aspirates), and autopsy procedures.
How?
1. Secure ties or elastic bands at middle of head and neck.
2. Fit flexible band to nose bridge.
3. Fit snug to face and below chin.
Sequence of Steps in a Particulate Respirator Fit Test
1. Cup the respirator in your hand with the nosepiece at your fingertips allowing the headbands to hang freely below your hand.
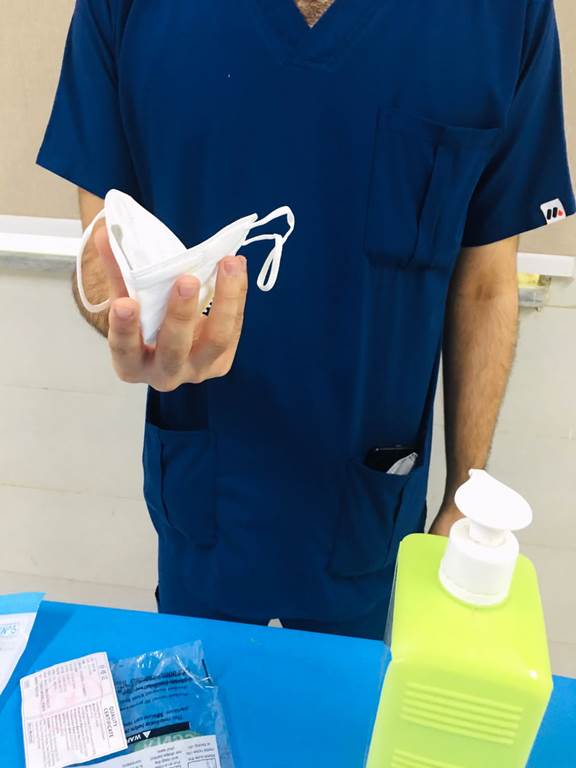
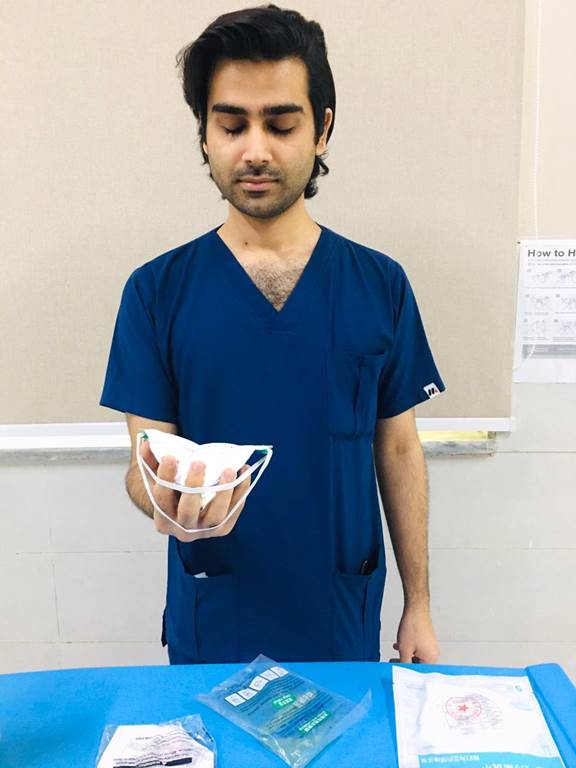
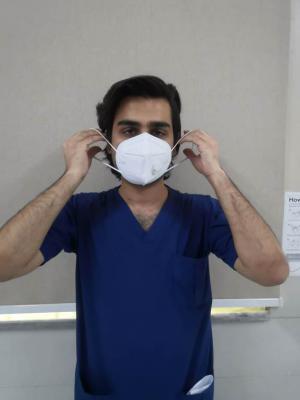
2. Position the respirator under your chin with the nosepiece up. Pull the top strap over your head resting it high at the back of your head. Pull the bottom strap over your head and position it around the back of neck below the ears.
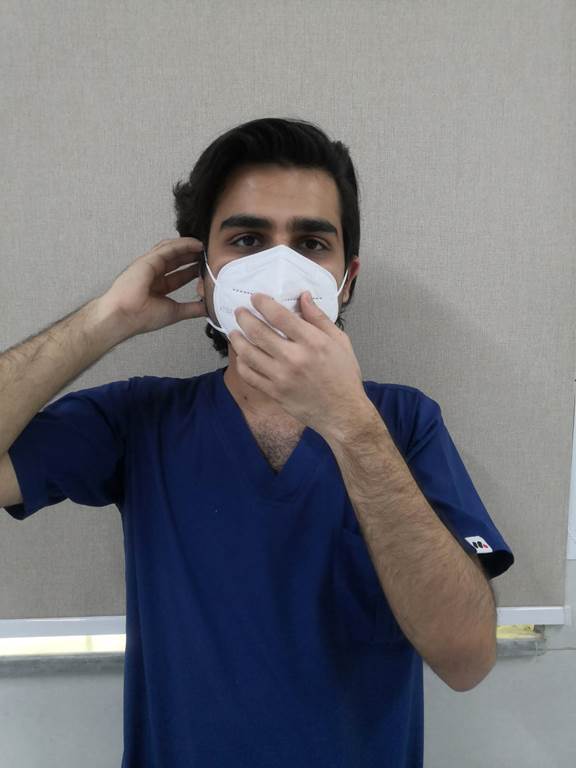
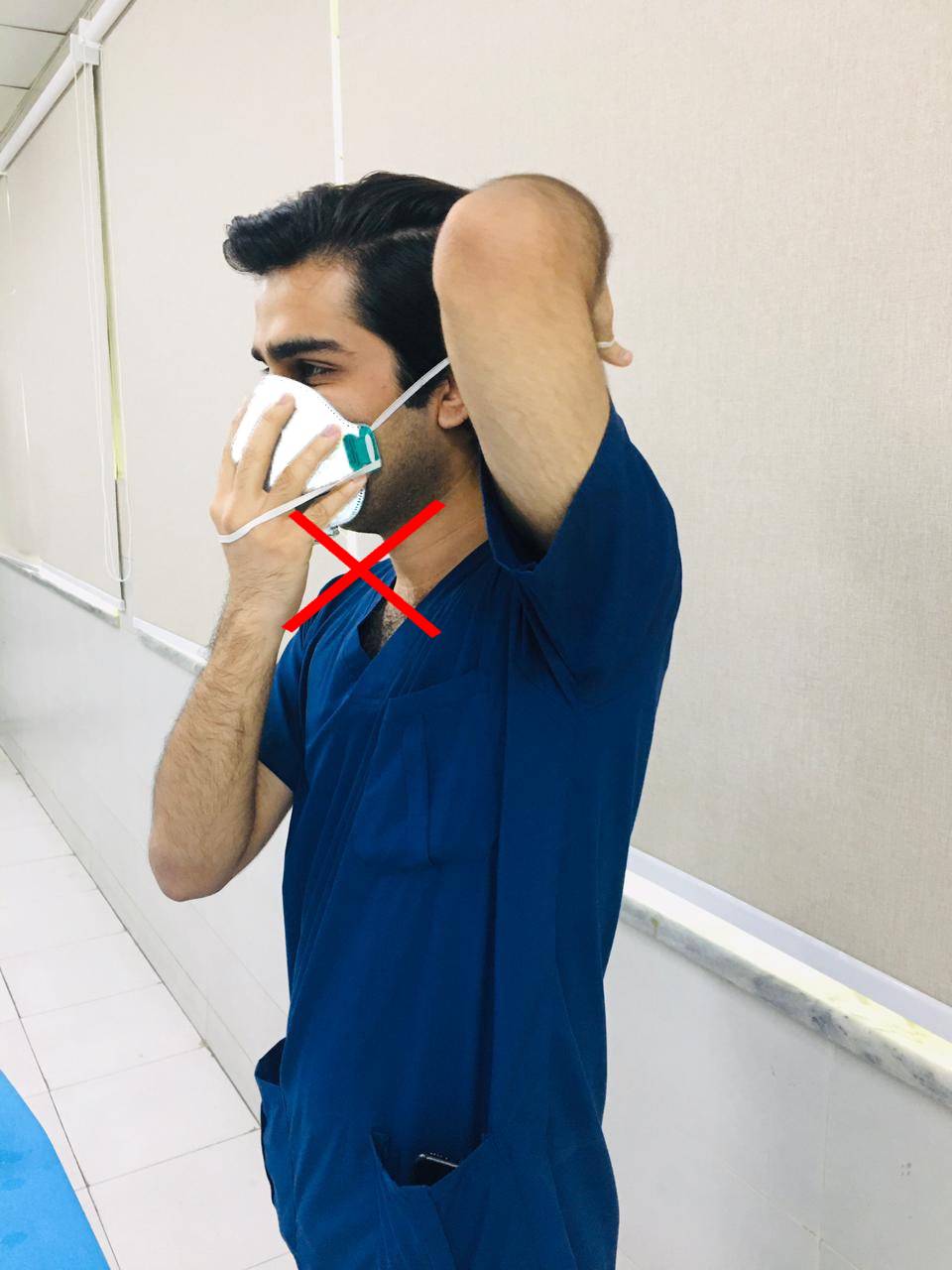
3. Place fingertips of both hand at the top of the metal nosepiece. Would the nosepiece (USING TWO FINGERS OF EACH HAND) to the shape of your nose. Pinching the nosepiece using one hand may result in less effective respirator performance.
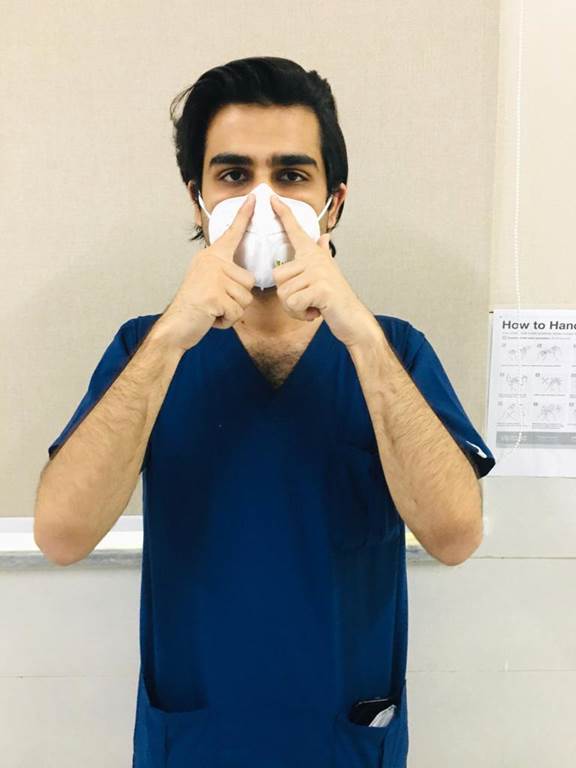
4. Cover the front of the respirator with both hands, being careful not to disturb the position of the respirator.
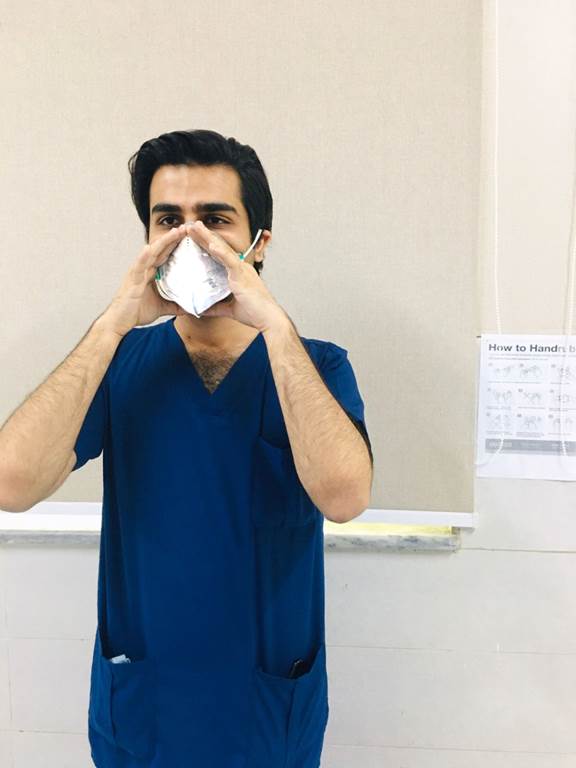
4A Positive Seal Check:
Exhale sharply. A positive pressure inside the respirator means no leakage. In case of leakage, adjust position and/or tension straps. Retest the seal.
4B Negative Seal Check:
Inhale deeply. In case of no leakage, negative pressure will make respirator cling to your face. Leakage will result in loss of negative pressure in the respirator due to air entering through gaps in the seal.
Warning
While doffing your respirator do not touch the front side. Remove N 95 by carefully pulling the straps away avoiding touching the surface of the mask.

Source: Infection prevention and control of epidemic and pandemic prone acute respiratory infection. Geneva: World Health Organization, 2014
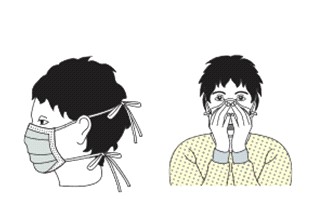
When
1. Wear eye protection/face protection (face shield or goggles) along with mask or respirator to protect the conjunctivae and the mucous membranes of the nose, eyes and mouth during activities that are likely to generate splashes or sprays of blood, body fluids, secretions, excretions or.
Aerosol Generating Procedures
1. Intubation, extubation, and related procedures, e.g. manual ventilation and open
airway suctioning (including tracheotomy care and open suctioning with invasive
ventilation).
2. Cardiopulmonary resuscitation.
3. Bronchoscopy (unless carried out through a closed- circuit ventilation system).
4. Surgery and post-mortem procedures in which high- speed devices are used.
5. Dental procedures.
6. Non-invasive ventilation (NIV), e.g. bi-level positive airway pressure ventilation (BiPAP).
7. Continuous positive airway pressure ventilation (CPAP)
8. High frequency oscillatory ventilation (HFOV).
9. Induction of sputum.
10. Collection of lower respiratory tract specimens (e.g. bronchial and tracheal aspirates), and autopsy procedures.
Source: Infection control precautions to minimise transmission of acute respiratory tract infections int healthcare settings. London: Public Healthcare England, 2016.
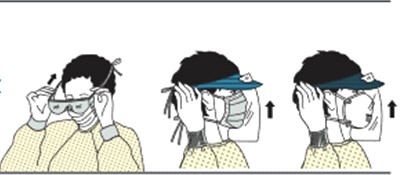
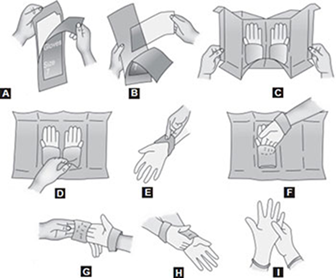
How?
Place over face and eyes and adjust to fit.
Hand hygiene should be performed before wearing and after taking off the gloves regardless of their type.
When
(For all surgical and aseptic procedures).
1. All surgical procedures/Vaginal delivery.
2. Performing Vascular access and procedures (central lines, IV line, urinary catheters, chest drain, etc).
3. Performing lumbar puncture, giving epidural, etc.
4. Invasive radiological procedures.
5. Preparing total parental nutrition and chemotherapeutic agents.
How?
When
(When risk of touching blood and body fluid or contact with microorganisms either from patients, items, equipment or the environment.)
1. Contact with not-intact skin or mucous membranes, e.g. vaginal or rectal examination, oral/dental care, emptying urinary bag, suctioning of endotracheal tubes.
2. Contact with potential presence of infectious against bot on intact and non-intact skin.
3. Indirect contact with blood and body fluids by handling and cleaning of contaminated items and equipment (emptying urine bag, emesis container etc.)
4. Handling of clinical/infectious waste.
5. Cleaning up spills of blood and body fluids.
How?
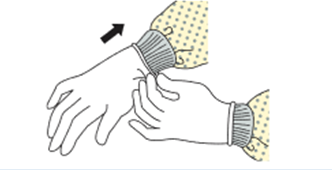
When
(No potential for exposure to blood or body fluids or contaminated environment).
1. Taking vitals (blood pressure, pulse, temperature).
2. Performing intra muscular and subcutaneous injections.
3. Giving oral medicines.
4. Vascular line manipulation in absence of blood leakage.
5. Using the telephone, writing in patient’s chart, moving patient’s furniture.

Source: Centers for Disease Control and Prevention (CDC)